Carbon Fiber Spine Instrumentation and the Role of Metal-Free Implants in Contemporary Spine Surgery
Advances in spine surgery are often defined by incremental refinements that improve precision, safety, and long-term decision-making. Implant materials are one such refinement. While titanium implants remain a durable and widely used standard in spinal fusion, carbon fiber–reinforced polymer instrumentation has emerged as a meaningful alternative in select clinical settings.
In Irvine, decisions regarding metal-free spine surgery are guided by clinical judgment rather than novelty. Dr. Hao-Hua Wu, MD, an orthopedic spine surgeon at UCI Health, incorporates carbon fiber spine instrumentation when its specific advantages—particularly in postoperative imaging and oncologic care—align with the patient’s diagnosis and long-term management plan.
Implant Material as a Deliberate Surgical Choice
Spinal implants must stabilize the vertebral column while bone fusion develops and neural structures remain protected. Titanium implants continue to serve this role effectively across anterior lumbar interbody fusion, posterior lumbar interbody fusion, transforaminal lumbar interbody fusion, lateral lumbar interbody fusion, and other interbody fusion techniques.
Dr. Wu does not approach implant selection as a routine preference. Instead, he evaluates the patient’s condition, imaging needs, and long-term surveillance requirements before recommending a specific construct. In patients where postoperative magnetic resonance imaging clarity is likely to influence care, carbon fiber instrumentation may offer meaningful advantages over traditional metal implants.
Carbon Fiber Spine Instrumentation in Irvine, CA
Carbon fiber spine instrumentation Irvine CA patients encounter in Dr. Wu’s practice reflects careful integration of biomechanics, imaging science, and surgical technique. Carbon fiber–reinforced implants are engineered to provide structural strength while exhibiting mechanical properties closer to cortical bone.
For Dr. Wu, the clinical significance lies less in the material itself and more in how it affects postoperative evaluation. Radiolucent implants allow clearer visualization of the spinal canal, spinal cord, nerve roots, disc space, intervertebral space, and adjacent vertebrae. This clarity supports more precise assessment of bony fusion, cage subsidence, spinal instability, and adjacent segment disease during follow-up.
In complex cases—such as revision spine surgery, infection, or spinal tumors—Dr. Wu may elect to use carbon fiber instrumentation specifically to preserve imaging quality for long-term monitoring.
Carbon Fiber Improves Postsurgical MRI Quality
Magnetic resonance imaging is central to modern spine care. It provides detailed evaluation of the spinal cord, nerve roots, and surrounding soft tissues in both the cervical spine and lumbar spine.
Dr. Wu routinely reviews postoperative MRI studies to assess decompression, evaluate new neurologic symptoms, and monitor patients who have undergone spinal fusion or interbody fusion. With traditional titanium implants, susceptibility artifact can partially obscure the spinal canal and limit visualization of neural structures. This can complicate interpretation, particularly in patients with complex pathology.
When carbon fiber instrumentation is used, postoperative MRI typically demonstrates substantially reduced artifact. In Dr. Wu’s experience, this improved visualization allows clearer assessment of the spinal cord and nerve roots after procedures such as anterior cervical discectomy, lumbar interbody fusion, or posterior interbody fusion. The ability to see neural elements more clearly supports confident clinical decision-making when patients present with new or evolving symptoms.
For patients who underwent lumbar interbody fusion and later require additional imaging, maintaining MRI clarity can be especially valuable in distinguishing normal postoperative changes from clinically significant findings.
Less Metal, Less Radiation for Spine Tumor Patients
In spine tumor surgery, imaging precision directly influences radiation planning. Dr. Wu treats both primary and metastatic spinal tumors within a multidisciplinary framework that includes radiation oncology.
When titanium implants are present, artifact on MRI and computed tomography can make it more challenging to delineate residual tumor from normal tissue. In cases where postoperative radiation therapy is anticipated, Dr. Wu may incorporate carbon fiber instrumentation to reduce imaging artifact and preserve clarity of the spinal canal and surrounding tissues.
Clearer imaging supports more precise radiation mapping. By improving target delineation, radiation oncologists can plan treatment with greater confidence while minimizing exposure to adjacent structures. In this way, implant selection becomes part of a coordinated oncologic strategy rather than a purely mechanical decision.
The imaging advantages of carbon fiber–reinforced instrumentation in spinal oncology are described in peer-reviewed literature, including an open-access study detailing navigation accuracy and multimodal imaging performance of carbon fiber–reinforced PEEK implants in spinal oncology (Navigation accuracy and assessability of carbon fiber-reinforced PEEK instrumentation with multimodal intraoperative imaging in spinal oncology, PubMed Central: https://pmc.ncbi.nlm.
Imaging Comparison in Spinal Oncology
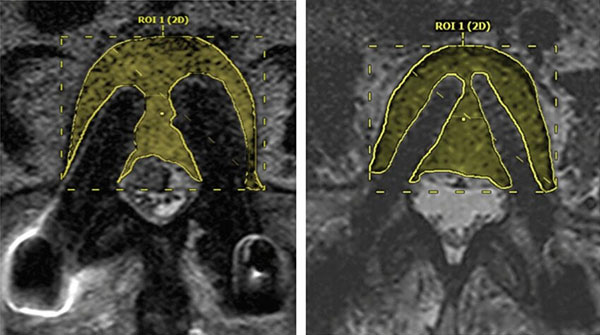
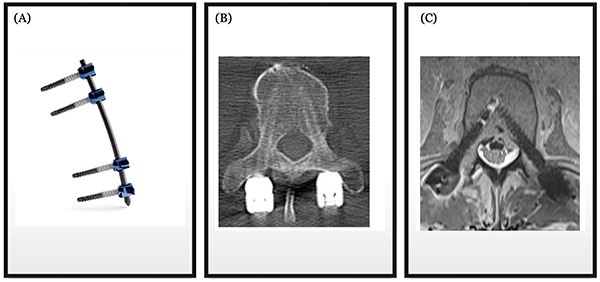
Representative imaging comparisons demonstrate reduced artifact with carbon fiber constructs relative to traditional metal implants. In Dr. Wu’s practice, this difference informs implant selection in patients where postoperative MRI surveillance or radiation planning is expected to be central to ongoing care.
Integration With Established Fusion Techniques
Carbon fiber instrumentation does not replace established spinal fusion procedures. Dr. Wu incorporates it into standard surgical methods when indicated, including anterior lumbar interbody fusion, posterior lumbar interbody fusion, transforaminal lumbar interbody fusion, and other lumbar fusion strategies.
During lumbar interbody fusion, restoration of disc space height and stabilization across the intervertebral space are critical. Expandable cages composed of carbon fiber can be used to achieve these objectives while maintaining radiographic visibility. This allows Dr. Wu to monitor bone graft incorporation, evaluate bone fusion, and assess alignment across adjacent vertebrae over time.
Similarly, in cervical procedures, reduced imaging artifact supports detailed evaluation of the spinal cord following decompression.
Minimally Invasive Spine Surgery and Precision Monitoring
Dr. Wu frequently utilizes minimally invasive spine surgery techniques when appropriate. Minimally invasive approaches aim to reduce disruption of surrounding tissues, limit blood loss, and preserve normal anatomy while achieving the same neurologic and mechanical goals as open surgery.
Carbon fiber instrumentation is compatible with minimally invasive techniques, including percutaneous fixation and selected standalone cage constructs. For Dr. Wu, the advantage lies in postoperative monitoring. Clear postoperative images allow careful evaluation of decompression, implant position, and fusion progression after minimally invasive surgery.
This is particularly relevant in patients with degenerative disc disease, lumbar spinal stenosis, or degenerative spondylolisthesis who undergo lumbar interbody fusion and require structured follow-up.
Long-Term Monitoring and Clinical Judgment
Spinal fusion depends on biologic healing. Bone graft placement, preservation of facet joints when appropriate, and stable fixation across the vertebral column remain central to achieving solid fusion. Carbon fiber implants do not alter these fundamentals.
Their value lies in how they support assessment over time. Dr. Wu closely monitors patients for adjacent segment disease, spinal instability, and signs of nonunion. Clear magnetic resonance imaging and computed tomography studies facilitate these evaluations, particularly in complex or oncologic cases.
Implant selection is therefore part of a broader strategy that prioritizes long-term function, protection of neural structures, and sustained quality of life.
Dr. Hao-Hua Wu’s Academic and Clinical Perspective
Dr. Hao-Hua Wu, MD, is a Harvard-trained orthopedic spine surgeon at UCI Health in Irvine, California. His clinical practice includes complex spine surgery, minimally invasive spine surgery, cervical and lumbar fusion procedures, spine tumor surgery, and advanced spinal implants such as carbon fiber instrumentation when clinically appropriate.
He is the founder of the Global Spine Research Initiative, the first academic global orthopaedic spine program in the United States, and leads international academic spine partnerships in Ethiopia, Nepal, Tanzania, and Ghana. His academic work includes more than 50 peer-reviewed publications in journals such as the Journal of Bone and Joint Surgery and the Journal of the American Association of Orthopaedic Surgeons.
Dr. Wu has been recognized with the national 2025 SpineLine “20 Under 40 Spine Surgeons” Award and was named a 2024 Top 20 Highest Rated Physician at UCI Health. These distinctions reflect peer recognition and patient experience within an academic medical environment.
Informed Spine Care in Irvine
For patients in Irvine considering spine surgery, discussions about implant materials are integrated into a comprehensive evaluation that includes diagnosis, treatment options, surgical technique, and long-term goals.
When imaging clarity, radiation planning precision, or complex postoperative monitoring are anticipated, Dr. Wu may incorporate carbon fiber spine instrumentation as part of a tailored surgical strategy. This measured approach reflects an emphasis on judgment, evidence-based care, and durable outcomes rather than routine adoption of new technology.










